Accreditation
Prepare and Apply
Here you will find all of the accreditation requirements, from preparing a program eligible for CPD credits to completing the application package.
Accreditation Requirements
Preparation should begin at least 3 months in advance. Plan to apply at least 6–8 weeks prior to start date as credits cannot be advertised prior to approval. Refer to the Overview page for important information on eligibility, processing times, application fees and credit types.
Read Documentation
Applicants should familiarize themselves with the following:
- UBC CPD Ethical Standards available for download: UBC CPD Ethical Standards for Accredited CPD Activities
- Steps for COI Management see UBC CPD Ethical Standards Appendix B
- Non-Compliance Procedure see UBC CPD Ethical Standards Appendix C
- Accreditation At-A-Glance: An infographic summarizing the accreditation responsibilities.
- Check the accreditation UPDATES for the most recent changes.
CHECKLIST & Forms
CHECKLIST for a complete application:
See more detailed descriptions further below under Planning Phases.
| Application Form to complete | ||
| Apply Online | Note: The fillable PDF application form has been discontinued. Please use the online application form link. | |
Signature Documents to submit Important: Remember to SAVE to your computer BEFORE completing or signing a fillable PDF | ||
| Disclosure Forms | Include disclosures of all SPC members with application. SPC members can use either version of the form: -Disclosure form (fillable PDF) If your Adobe version does not have a Portfolio function to combine signed docs, please forward the individual disclosures via email to cpd.accreditation(at)ubc.ca. -Online disclosure form (link) A copy of responses will be emailed to the individual user, as well as to your SPC Chair for review. You will need to provide users with an email contact for your SPC Chair . | |
| Declaration Forms | A few SPC members are required to take on a formal role(s) defined by credit type and formalized via declaration. There are 2-4 possible roles depending on application type. A qualifying physician may take on more than one role: -Accountable physician required for all credit types -RCSPC physician for MOC credits -CFPC physician and UBC FoM physician (same form) for Mainpro+ | |
| Program Materials to submit | ||
| Needs Assessment Tools | Eg. previous evaluation summary, survey results, etc. Needs Assessment (sample) | |
| Budget | Budget that identifies all funding sources and general expenses. If internally funded, state the org/dept name on the budget. Indicate how any surplus or deficit will be handled. See Budget (sample) | |
| Program Agenda | Detailed program agenda, including learner-centred objectives, and start and end times and breaks is needed for accurate credit count. See Agenda (sample) Submit any program marketing such as brochure/flyer or invitation email, links to website, registration, etc. The physician organization must be clearly identifiable on all educational materials. | |
| Speaker Communications | The SPC must inform anyone contributing to CPD activity content of their responsibilities regarding accreditation standards. This is informally known as "Speaker Comms" or "Speaker Letter", but applies to all content contributors (speakers, moderators, facilitators, and authors) Speaker Comms (sample) | |
| Evaluation Form | Incorporate requirements into your existing program evaluation strategy: -Program evaluation - required questions -Speaker evaluation (optional) | |
| Certificate | Certificate (sample) | |
Additional requirement for assessment programs: | ||
| Assessment Tool | Required for assessment credits: Tool used to objectively assess the learner's knowledge or performance e.g. quiz, skills checklist, etc. | |
| Reflective Tool (Optional) | Reflective Tool (optional) | |
Additional requirements for commercially sponsored programs: | ||
| Sponsorship Prospectus & Agreement | Required only for programs seeking commercial sponsorship: -Sponsorship Agreement (sample) -Sponsorship Prospectus/Invite (sample) | |
Apply Here
Apply once your program has been fully developed and before you begin any advertising.
The application fee is due at the time of application.
To preview the application questions, click Apply Online or download the application questions only document.
To complete the online application, click Apply Online. Select Save Progress once to generate a unique URL and activate auto‑save. Bookmark this URL so you can return to your application later or share it with others who need to contribute. Upload all required program materials and signed documents directly in the form. Once everything is complete, click Submit to be taken to the payment page.
If you are new to accreditation, the Planning Phases section below integrates accreditation standards into a process for planning a CPD program that is eligible for accreditation:
Planning Phases
Submitting an application is only one step in the accreditation process. To be successful, your program must have proper governance and be planned and developed in alignment with accreditation standards (ethical, educational, administrative) from the start.
The planning phases below expand on the checklist.
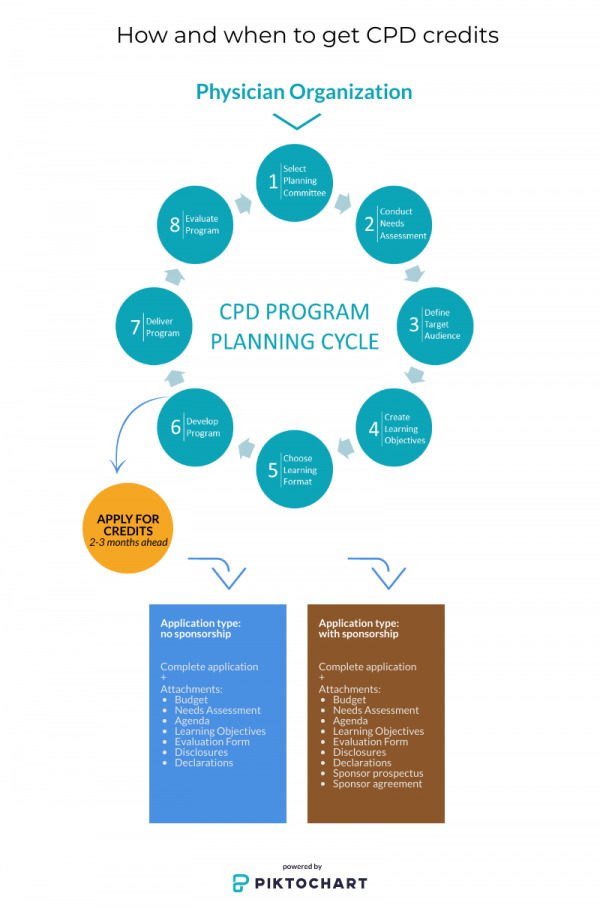
 Physician Organization
Physician Organization
Governance
Only a physician organization may seek accreditation. Every CPD activity must be clearly developed by a physician organization accountable for all aspects of the CPD activity, including finances. The physician organization must make all decisions regarding the receipt and disbursement of all funds in line with the UBC CPD Ethical Standards.
Definition
A physician organization is a not-for-profit group of health professionals with a formal governance structure, accountable to and serving, among others, its physician members through continuing professional development, provision of healthcare and/or research.
Eligibility and Membership Criteria
- The organization has been formally established for at least one year.
- Members are physicians.
- Membership extends beyond the Board of Directors.
- Membership extends beyond receiving a newsletter.
- Defined criteria exist for member eligibility.
- Clear expectations are outlined for members (e.g., payment of dues).
- Members have voting rights on the organization’s strategic directions and initiatives.
Examples include the following:
- Faculties of medicine
- Hospital departments or divisions
- Medical societies
- Medical associations
- Medical academies
- Physician research organizations
- Physician clinics
- Health authority medical department or medical advisory committee (HAMAC)
- Canadian provincial medical regulatory authorities (MRAs)
This definition does NOT include:
- Healthcare/pharmaceutical industry commercial interests (HPIs)
- Health authority administration offices
- Disease-oriented patient advocacy organizations (e.g. Canadian Diabetes Association)
- Government departments or agencies (e.g. Health Canada, Public Health Agency of Canada)
- Small number of physicians working together to develop educational programming
Please note: Organizations who have not applied before may need to provide supporting documentation demonstrating the organization meets the required criteria (e.g. Terms of Reference, constitution, meeting minutes, constitution, governance policies, etc ). This may increase application processing time beyond the typical 4-6 weeks.
Co-development
FOR MOC ONLY
Co-development is the process by which two or more not-for-profit organizations — at least one of which must be the physician organization — prospectively collaborate to develop content. Although some responsibilities may be delegated to the co-developing organization, the physician organization must assume control over all aspects as if they were planning the event independently.
Co-development may or may not include financial support; however, for-profit organizations cannot be co-developers.
 Scientific Planning Committee (SPC)
Scientific Planning Committee (SPC)
Every CPD activity must have a scientific planning committee (SPC), accountable to and overseen by a fiscally responsible physician organization. The SPC is responsible for protecting the CPD learning environment and program content/quality. The SPC must follow the UBC CPD Ethical Standards for all aspects of the CPD activity and ensure that the CPD activity is not used to promote or sell products or services that serve any form of professional or financial interests, including their own.
The SPC must (i) include at least two physicians and (ii) be representative of the target audience. Members must be aware of their responsibilities pertaining to accreditation/certification standards. The SPC must have a chair and an agreed decision-making process to enable it to fulfill its responsibilities.
Disclosures (from each SPC member) and declarations (for specific SPC member roles) need to be signed and submitted with application. See below.
Responsibilities of SPC
- Uphold the UBC CPD Ethical Standards for all aspects of the CPD activity
- Identify the educational needs of the intended target audience
- Develop learning objectives
- Select educational methods
- Select SPC members, speakers, moderators, facilitators and/or authors
- Develop and deliver content
- Evaluate outcomes
- Oversee logistics
- Review disclosures and mitigate conflicts of interest
- Ensure commercial sponsorship support and programming comply with standards
SPC members should familiarize themselves with the accreditation standards:
- Ethical Standards including disclosure review and conflict of interest (COI) management:
- Disclosures for identifying COIs
- Steps for COI Management see Ethical Standards Appendix B
- Non-Compliance Procedures see Ethical Standards Appendix C
- Informing presenters and others of their responsibilities ('speaker letter')
- Educational Standards for MOC and/or Mainpro+ credits, including
- Declarations for SPC roles related to credit type
- Accreditation At-A-Glance: An infographic summarizing physician organization and SPC accountability
NOTE: Representatives of Healthcare and/or Pharmaceutical Industry (HPI) companies cannot be members of the SPC or participate in decisions related to any aspect of the CPD activity.
 Declarations
Declarations
Consult CHECKLIST & Forms to access the appropriate Declaration Forms.
Declarations are required by select SPC members who qualify to take on a formal role for the credit type. A qualifying physician may have more than one SPC role (eg. one could serve as accountable physician and RCSPC member).
Accountable Physician
Required for all programs. The accountable physician is the chair or one member of the SPC representing the physician organization, and as such agrees to assume ultimate responsibility for upholding the accreditation/certification standards and for following the UBC CPD Guidelines for Support in preparing and implementing the CPD activity.
RCPSC Member
Required for MOC credits. One physician member of the Royal College of Physicians and Surgeons of Canada (RCPSC) is required to be on the SPC to represent the target audience of specialists. The declaration verifies the RCPSC member of having had substantial input into the program.
UBC FoM Member
Required for Mainpro+ credits. UBC CPD can only certify UBC Faculty of Medicine (UBC FoM) Activities for Mainpro+ credits. A UBC FoM physician member is required to be on the SPC and must have substantial involvement in the program for it to be considered a UBC Activity.
CFPC Member
Required for Mainpro+ credits. One physician member of the College of Family Physicians of Canada (CFPC), residing in the province of BC, is required to be on the SPC to represent the target audience of BC family physicians.
 Disclosures
Disclosures
A conflict of interest (COI) occurs when external interests interfere or appear to interfere with the primary interest - in this case an accredited CPD activity. The global best practice in CPD is for all individuals involved in developing accredited CPD activities to be transparent about their financial relationships through a disclosure process, outlined below.
Disclosure Review Process
- Collect SPC members' disclosures and include with your accreditation application.
- Collect content contributors' disclosures (presenters, authors, instructional designers, facilitators, moderators, etc.) for your SPC to review. These do not need to be submitted to UBC CPD.
- Communicate all disclosures to learners. Once the review concludes that there are no conflicts of interest (COI), ensure the remaining relevant financial relationships are disclosed to participants for transparency. See Disclosure-Summary.
Note speakers are required to disclose both written (slide) and verbally.
COI Management
The SPC members are responsible to review each others' disclosures and the disclosures of all content contributors to eliminate unresolvable financial relationships and mitigate relevant financial relationships. A step-by-step review process is available in the UBC CPD Ethical Standards, Element 3.0.
Disclosure Form
See the CHECKLIST & Forms for the disclosure form.
 Define Target Audience
Define Target Audience
For CPD activities to be eligible for accreditation, the PRIMARY target audience must be physicians (specialists, family physicians, or both). Aside from governing the program design and content, identifying the target audience determines which type of credits will be most appropriate. You can look up individual physicians in the provincial regulatory college directory (or either national medical college) to verify what kind of medicine they are certified to practice in BC: https://www.cpsbc.ca/public/registrant-directory
| RCPSC Specialists (MOC credits) | CFPC Family Physicians (Mainpro+ credits) |
|---|---|
| Acute Care Point of Care Ultrasonography (POCUS) Addiction Medicine Adolescent and Young Adult (AYA) Oncology Adolescent Medicine Adult Cardiac Electrophysiology Adult Echocardiography Adult Hepatology Adult Interventional Cardiology Adult Thrombosis Medicine Advanced Heart Failure and Cardiac Transplantation Aerospace Medicine Anatomical Pathology Anesthesiology Brachytherapy Cardiac Surgery Cardiology (adult or pediatrics) Child and Adolescent Psychiatry Child Maltreatment Pediatrics Clinical Immunology & Allergy (adult or pediatrics) Clinical Pharmacology & Toxicology Clinician Educator Clinician Investigator Program Colorectal Surgery Critical Care Medicine (adult or pediatrics) Cytopathology Dermatology Developmental Pediatrics Diagnostic Radiology Emergency Medical Services Emergency Medicine Endocrinology & Metabolism (adult or pediatrics) Forensic Pathology Forensic Psychiatry Gastroenterology (adult or pediatrics) General Internal Medicine General Pathology General Surgery General Surgical Oncology Geriatric Medicine Geriatric Psychiatry Gynecologic Oncology Gynecologic Reproductive Endocrinology & Infertility Hematological Pathology Hematology Hyperbaric Medicine Infectious Diseases (adult or pediatrics) Internal Medicine Interventional Radiology Maternal Fetal Medicine Medical Biochemistry Medical Genetics and Genomics Medical Microbiology Medical Oncology Neonatal Perinatal Medicine Nephrology (adult or pediatrics) Neurology (adult or pediatrics) Neuropathology Neuroradiology Neurosurgery Nuclear Medicine Obstetrics & Gynecology Occupational Medicine Ophthalmology Orthopedic Surgery Otolaryngology - Head and Neck Surgery Pain Medicine Palliative Medicine Patient Safety and Quality Improvement Pediatric Emergency Medicine Pediatric Hematology/Oncology Pediatric Radiology Pediatric Surgery Pediatric Urology Pediatrics Physical Medicine & Rehabilitation Plastic Surgery Psychiatry Public Health and Preventive Medicine Radiation Oncology Respirology (adult or pediatrics) Rheumatology (adult or pediatrics) Sleep Disorder Medicine Solid Organ Transplantation Sport and Exercise Medicine Surgical Foundations Thoracic Surgery Transfusion Medicine Trauma General Surgery Urology Vascular Surgery Other/General Practice/Health Care Professional Royal College of Physicians and Surgeons of Canada Canadian Medical Protective Association | Aboriginal health
|
 Conduct Needs Assessment
Conduct Needs Assessment
Needs assessment is the process involved in gathering information to identify the learning needs of the target audience. The learning needs are the basis for identifying appropriate learning objectives and the content and format of the educational activity. To identify the learning gap the SPC should describe the target audience, work environment or work activities, and demonstrate a valid professional practice gap from which the educational needs are identified. Identify preferred learning style and current knowledge or skill level, then determine desired knowledge or skill level.
The most useful needs assessments are those where multiple methods are utilized to identify educational needs linked to improved patient care.
To help identify needs, the SPC should ask the following questions:
- How common is the need among our target audience?
- How many different assessment sources indicate this need?
- How significantly will the unfulfilled learning need hinder health care delivery?
- How directly is the need related to actual physician performance?
- How likely is it that a CPD activity will improve practice behaviour?
- Are sufficient resources available to effectively address this topic?
- How receptive will our target audience be to a session on this topic?
NOTE: Since the release of the National Standard released in Jan 2018, needs assessment tools are required to be submitted with an application (examples include past evaluations, focus group questionnaires etc.).
See the CHECKLIST & Forms for a sample needs assessment.
 Address CanMEDS Roles
Address CanMEDS Roles
To be eligible for accreditation, a program must address at least one of the seven roles by tying them to the learning objectives.
The CanMEDS and CanMEDS-FM competencies are frameworks developed by the Canadian medical colleges. They identify and describe the abilities physicians and surgeons require to effectively meet the health-care needs of the people they serve. These abilities are grouped thematically under the seven roles of a physician.
| ROLE | Description | |
|---|---|---|
| Medical Expert/ ExpertFM | Medical Expertise | As Experts, physicians integrate all of the roles, applying medical knowledge, clinical skills, and professional attitudes in their provision of patient-centered care. Central physician role in framework. |
| Communicator | Communicating with Patients | As Communicators, physicians effectively facilitate the doctor-patient relationship and the dynamic exchanges that occur before, during, and after the medical encounter. |
| Collaborator | Collaborating with Colleagues | As Collaborators, physicians effectively work within a healthcare team to achieve optimal patient care. |
| Leader/ManagerFM | Coordinating Team Care | As Managers, physicians are integral participants in healthcare organizations, organizing sustainable practices, making decisions about allocating resources, and contributing to the effectiveness of the healthcare system. |
| Health Advocate | Advocating for Improved Care | As Health Advocates, physicians responsibly use their expertise and influence to advance the health and well-being of individual patients, communities, and populations. |
| Scholar | Contributing to Medical Academic Knowledge Domain | As Scholars, physicians demonstrate a lifelong commitment to reflective learning, as well as the creation, dissemination, application and translation of medical knowledge. |
| Professional | Accountability and Ethical Practice | As Professionals, physicians are committed to the health and well-being of individuals and society through ethical practice, profession-led regulation, and high personal standards of behaviour. |
Historical context: The term CanMEDS initially stood for the Canadian Medical Education Directives for Specialists; CanMEDS-FM was later incorporated to include family physicians as well.
 Financial Accountability
Financial Accountability
The physician organization must have overall accountability for the finances of the CPD activity. This means that all funds must be paid to and expenses paid by the physician organization.
Accredited activities should aim to be financially self-sustaining, and should not be profit-generating. Surplus funds generated from a recurring activity should be earmarked for the planning, development, or delivery of subsequent activities of a recurring nature. Surplus funds from a single, non-recurring event should be returned to the physician organization (not an individual) and be used to support continuing education activities in the organization.
Create a Budget
Identify all sources of funding/revenue and expenses directly on the budget, even if internally funded. Indicate how any surplus or deficit will be handled. A budget with all projected revenues/funding from all sources, and general expenses, is to be submitted with the application package.
See the CHECKLIST & Forms for a sample budget.
Sponsorship
If you are planning to obtain sponsorship, please follow the UBC CPD Ethical Standards for Accredited CPD Activities 2024, Element 4. Remember that commercial sponsorship requires that participants be charged registration fees.
Only the UBC CPD-approved sponsorship opportunities may be offered. The terms, conditions and purposes by which commercial sponsorship is provided must be documented in a written agreement that is signed by the CPD provider organization and for-profit sponsors. The sponsorship agreement reflects the sponsorship request/prospectus.
See CHECKLIST & Forms for: Sponsorship Agreement
 Sponsorship
Sponsorship
 Choose Learning Format
Choose Learning Format
As of December 16, 2024, there have been significant changes to the CFPC credit framework. The new Mainpro+ credit types are described below, but essentially the credit type Mainpro+ Certified now covers all eligible learning formats (group leaning, online modules, knowledge assessments and simulation).
| Credit System | Credit Type UBC CPD can provide | Credit Description |
|---|---|---|
| Royal College (MOC) | MOC Section 1 Group Learning | Interactive learning (workshops, conferences, live webinars); ≥25% group interactivity. May be synchronous (live, in-person or virtual) or asynchronous (eg. interaction via facilitated discussion board) |
| MOC Section 3 SAP | Structured knowledge assessment with individualized feedback (eg. eLearning modules). Provides learner with individualized, objective feedback on their knowledge, includes: - correct and incorrect answers, plus explanations of why they are correct/incorrect, and - a scored assessment, and - suggested further resources for more information No group interactivity required | |
| MOC Section 3 SIM | Structured performance assessment with individualized feedback (eg. simulation scenarios). Provides learner with individualized, objective feedback on their performance (eg. via instructor's skills checklist). to enable the identification of any area(s) requiring improvement through development of a future learning plan. No group interactivity required. | |
| CFPC (Mainpro+) | Mainpro+ Certified | Program design may be either group interactivity or structured assessment. Corresponds to any of the above MOC credit types. |
| Mainpro+ Certified Assessment | For practice‑assessment activities ONLY. Must include all of the following: 1. Learners reflect on current practice; 2. Learner receive objective feedback (data) that compares their practice to expected standards; 3. Learners reflect on changes to their practice; 4. Learners report back on changes made to their practice Does not correspond to any of the above MOC credit types. |
Note: Available MOC credits have not changed.
 Create Learning Objectives
Create Learning Objectives
Learning objectives that address identified needs must be created for the overall event and for individual sessions, and be available to participants. A learner-centered objective is specific, short-range, and relatively concrete. It describes what a learner will be able to do differently afterward (what learner behaviour will change).
Learner Centered Objectives
The change in behaviour is characterized by the use of an action verb. Crystalize the intent of your sessions by reviewing the list of action verbs.
“What will the learner be able to DO once learning has occurred?”
Eg:
Identify the inflammatory markers in AMD.
Recognize the predictors of diabetic retinopathy.
Describe the process of fluid detection by OCT.
Appraise difficult cases presented by members.
TIP: Avoid the use of vague verbs such as understand, know, appreciate, familiarize, gain knowledge of, grasp, be aware of, comprehend, appreciate, study, become acquainted with or learn about.
CanMEDS/CanMEDS-FM
The CanMEDS and CanMEDS-FM competencies are frameworks developed by the Canadian medical colleges. They identify and describe the abilities physicians and surgeons require to effectively meet the health-care needs of the people they serve. These abilities are grouped thematically under the seven roles of a physician.
To help ensure that CPD learning activities and programs are aligned with CanMEDS, learning objectives should address one or two of the seven roles.
| CanMEDS Role | Description |
|---|---|
| Medical/Family medicine expert | Medical expertise |
| Communicator | Communicating with patients |
| Collaborator | Collaborating with colleagues |
| Leader | Coordinating team care |
| Health advocate | Advocating for improved care |
| Scholar | Contributing to medical academic knowledge domain |
| Professional | Accountability and ethical practice |
 Develop Content
Develop Content
Design your CPD learning activity to address the professional practice gaps identified by the needs assessment.
Create a detailed program with an agenda of topics, speakers, start and end times, question and answer/discussion periods, breaks, etc.
- Include the learner-centred objectives in the program
- Count credit hours by totaling the educational hours and subtracting the breaks
- Ensure the physician organization accountable for the program is clearly identifiable on all educational materials
- Relay the accreditation standards to all those developing content ("speaker communications")
Consult CHECKLIST & Forms for template
Non-Compliance Procedures
The SPC must identify and address instances of non-compliance with the UBC CPD Ethical Standard 2024. The SPC must have a procedure for addressing non-compliance; where no other procedure exists, the UBC CPD Non-Compliance Procedures (see Appendix C) may be used. The SPC must inform UBC CPD should any instances of non-compliance arise.
 Speaker Letter
Speaker Letter
Inform Content contributors of Accreditation standards
The SPC must inform content contributors (e.g. presenters, authors, instructional designers, facilitators, moderators, etc.) of the requirements to:
- develop content and learning objectives based on the identified needs of the target audience [note: SPC should share identified needs with content contributors]
- develop learning objectives that are learner-centred
- create content and materials that provide (where applicable) a balanced view for therapeutic options related to the content area and reflect the current scientific literature
- describe therapeutic options using generic names (or both generic and trade) and not reflect exclusivity and branding
- declare any off-label use when making therapeutic recommendations for medications that have not received regulatory approval
- make every effort to avoid bias, whether commercial or other
- disclose all financial relationships with commercial and not-for-profit organizations
- presenters must disclose to learners both on slides and verbally
- include references to evidence used to create content
- adhere to time allotment, including time for interactivity such as Q & A
- ensure content and materials are available to the SPC for review prior to being made available to learners
- ensure content and materials meet professional standards and legal requirements, including the protection of privacy, confidentiality and copyright
Consult CHECKLIST & Forms to access the speaker communication (comms) template.
 Apply Now
Apply Now
By now your program is ready to be reviewed for CPD credit approval.
Consult the CHECKLIST & Forms to ensure you have all of the required documentation and apply.
Applying via the online portal under Apply Here.
 Deliver Program
Deliver Program
Once your program has been approved, you will receive an approval email with your official accreditation/certification statement to be used on certificates and in marketing materials. UBC CPD forwards notification of approval of your activity to the appropriate medical college(s) so that physician may claim credits after attending.
Registration
All participants must be able to register and receive a receipt or record of registration. Keep attendance records for 6 years.
Certificates
A certificate of participation or written confirmation signed by the chair of the SPC is to be issued to physician participants for all accredited/certified activities. To claim credits, physicians log into their member portal with the Royal College or the CFPC.
Certificates may be issued to any participants as proof of participation, even if they are not physicians. Health professionals such as nurses and midwives especially use these certificates to track their own CPD.
See the CHECKLIST & Forms for: Certificate template.
The certificate must specify the following elements:
- Participant name
- The title of the activity as it appears on the application
- The name/logo of the physician organization accountable for the CPD activity must be clearly visible
- The date(s) the activity took place
- The location of the activity (i.e. city, prov or virtual base)
- Accreditation/certification statement issued upon approval, including number of CPD credits
- Signature of the SPC Chair/Accountable Physician (preferred)
- Cert+ session ID (Mainpro+ only)
A NOTE ON MAINPRO+ SESSION IDs
For series: You can specify in your application if you will be distributing certificates after each session or one certificate at the end. Either is fine, just keep in mind that it is easier on all sides, including for physicians claiming the credits, if there is one certificate - but both options are available.
 Evaluate Program
Evaluate Program
Evaluation allows for the ongoing improvement of CPD programs and provides valuable feedback to program planners and faculty, and is a mandatory component of all accredited/certified programs. Learners must be provided with an opportunity to evaluate the CPD activity in a meaningful and confidential manner (but should not be required to complete an evaluation in order to obtain their CPD credits).
Required evaluation questions
Please incorporate the following required evaluation questions into your existing evaluation strategy. NOTE: The first three questions are required for all programs; the rest are only required for specific credit/content types:
- Did the program meet the stated learning objectives? Strongly disagree Disagree Neutral Agree Strongly agree
Required wording for Mainpro+ credits: As a result of completing this CPD activity I am confident in my ability to achieve the learning objectives. Strongly disagree Disagree Neutral Agree Strongly agree
- Were there any aspects of the program's content or delivery that appeared biased to you (e.g. financial, sponsor-related, cultural, gender, racial, or others)? Yes No | If yes, please describe: ___
Alternative option: Did you perceive any degree of bias in this program or its delivery in either of the following categories: a) Bias towards external interests (financial or sponsor-related) Yes No | If yes, please describe: ___ b) Bias for or against specific communities or groups (cultural, gender, racial or other) Yes No | If yes, please describe: ___
- Reflecting on the program content, what impact will this education have on your practice? Open text box
- Required only if content covers treatments, medications, devices, etc. This education offered balanced views of diagnostic tools and/or therapeutic options. Strongly disagree Disagree Neutral Agree Strongly agree
- Required for MOC credits: Which CanMEDS Role(s) were addressed during this CPD activity? Check all that apply: ☐ Medical Expert ☐ Communicator ☐ Collaborator ☐ Leader ☐ Health Advocate ☐ Professional ☐ Scholar
See the CHECKLIST & Forms for: Evaluation templates.
Evaluation considerations
The following question can be used as a needs assessment for future activities:
- Please suggest any topics or speakers you would like to see at future CPD activities. Open text box
If elements promoting Equity, Diversity, and Inclusion are considered in the program planning (e.g. including diverse and varied perspectives in planning, considering diverse needs of learners and patients they treat, implementing an inclusive program design, considering accommodations for learners), remember to provide learners an opportunity to evaluate how well the program incorporated EDI principles.
Dropped evaluation questions for Mainpro+
As of December 2024, the CFPC dropped the Quality Criteria that was Addressing Barriers , therefore this evaluation question is no longer required:
- Can you identify any barriers to incorporating what you learned into your practice?
As of June 2018, these two questions are no longer required on evaluations for Mainpro+ programs:
- This CPD activity content enhanced my knowledge
- Indicate which CanMEDS-FM roles you felt were addressed Note: the CanMEDS question is still required for MOC accreditation!
 Report Back
Report Back
The evaluation must include the question: “Did you perceive any degree of bias in any part of the program? Yes/No”. The responses to this question (ie. the number of yes, no and total responses) are to be forwarded to UBC CPD within 3 months of the event, via a brief email.